Lab 10: The Urinary System - Anatomy
Table of Contents
Preparation for lab
To get the most out of this lab you need to be prepared. The basic knowledge needed for this lab is covered
- In the reading on the rest of the page.
- In Amerman “Human Anatomy and Physiology” in Chapter 24 “The Urinary System”.
- In OpenStax Chapter 25 The Urinary System.
Learning outcomes of the lab exercises:
- Identify the structures and organs of the urinary system.
- Define the main function of each of the urinary system organs.
- Compare and contrast the histological features of the tissues in the urinary system.
Today’s Activities
- Kidney dissection
- Urinarlysis (optional)
- Complete the lab report.
Overview
The urinary system is the body’s filtration and waste-removal network, responsible for maintaining fluid balance, electrolyte levels, and overall internal stability. It consists of the kidneys, ureters, urinary bladder, and urethra: the kidneys filter the blood to remove waste products and excess substances, producing urine; the ureters transport this urine to the bladder, where it is stored; and the urethra carries it out of the body during urination. Along the way, the system helps regulate blood pressure, pH balance, and red blood cell production through hormone release, making it essential not just for waste elimination but for overall homeostasis.
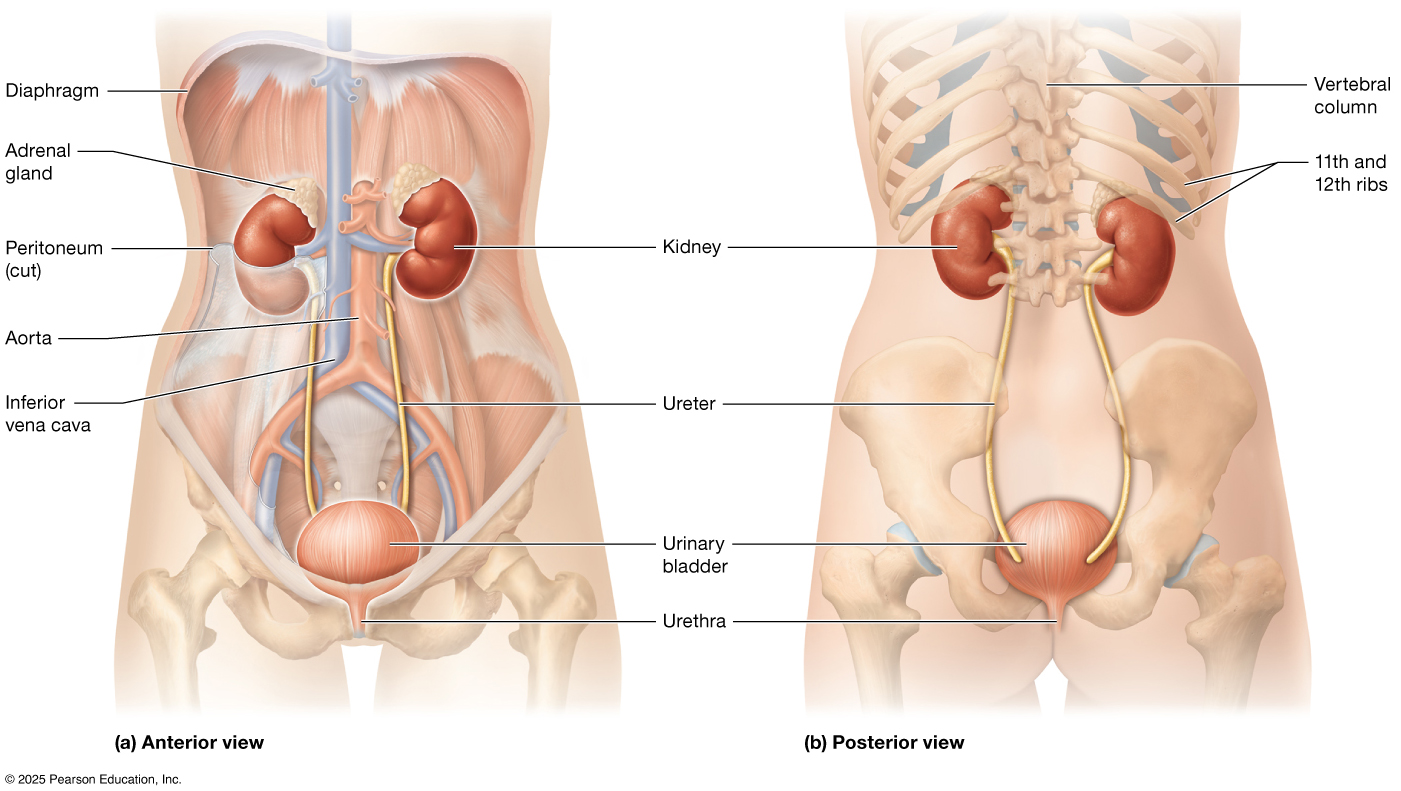
The Structures of the Urinary System
Kidney
The kidney is a bean-shaped organ located in the abdominal cavity in a retroperitoneal position, meaning it sits behind the peritoneum along the posterior body wall. Each kidney is enclosed by a tough, fibrous renal capsule that helps protect it and maintain its shape. On the medial side is an indentation called the hilum, where three structures enter and exit: the renal artery, which brings unfiltered, oxygenated blood into the kidney; the renal vein, which carries filtered, deoxygenated blood away; and the ureter, which allows urine to flow out of the kidney toward the urinary bladder.
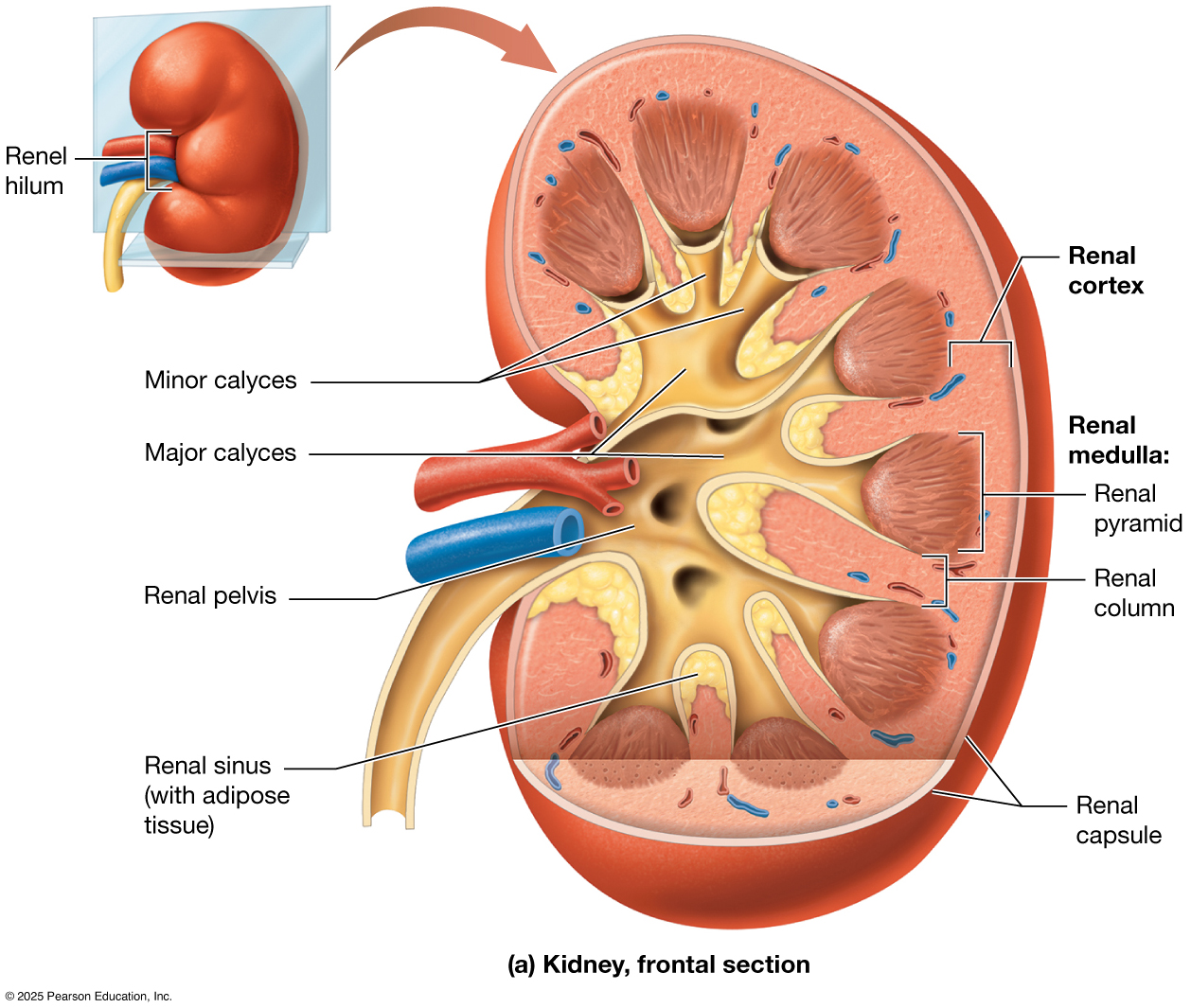
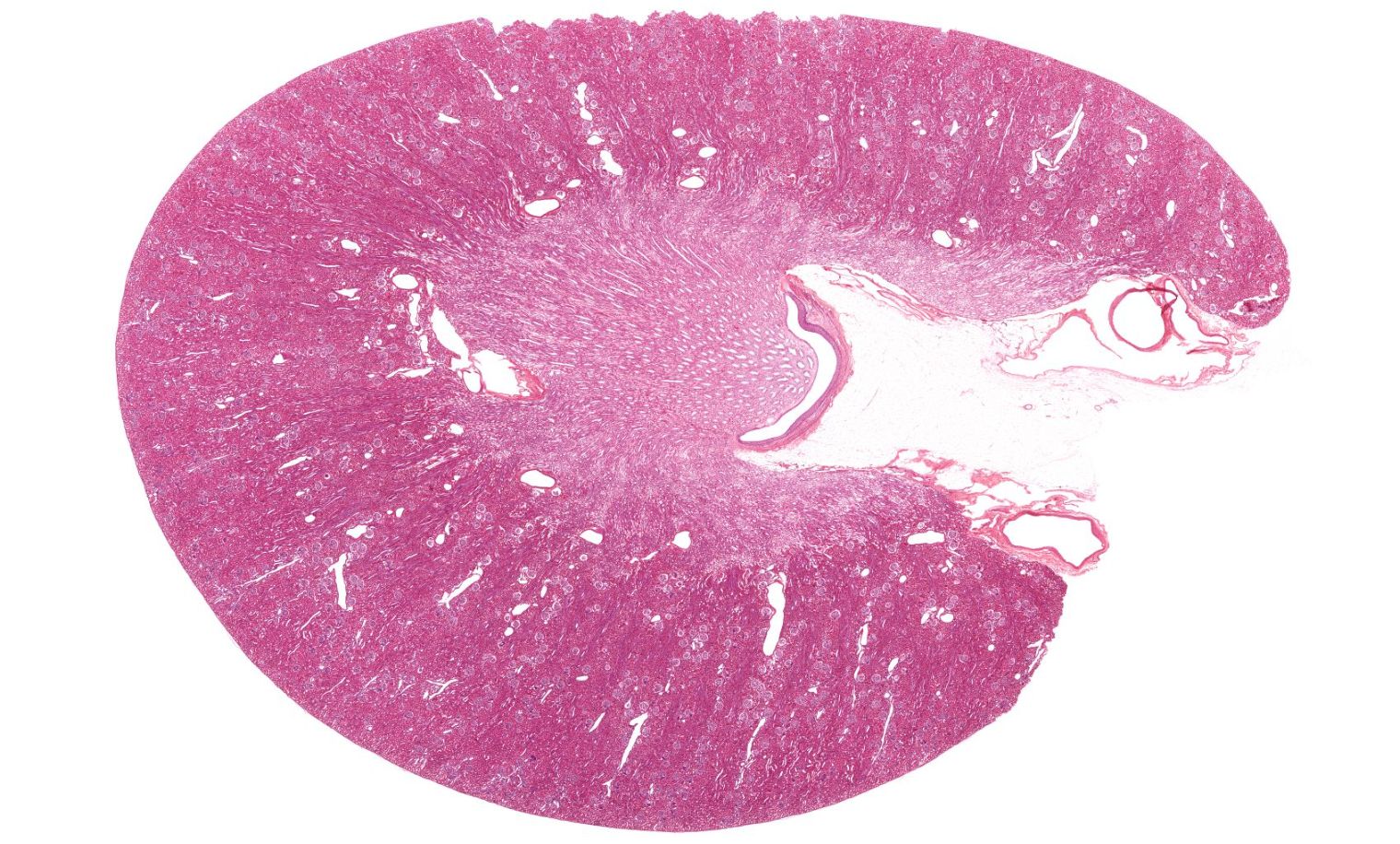
Internally, the kidney is divided into two main regions: the outer cortex and the inner medulla. The medulla contains cone-shaped structures called renal pyramids, which are separated by extensions of cortical tissue known as renal columns. Urine produced in the nephron passes first into the collecting duct and then into small collecting spaces called minor calyces, which merge to form larger major calyces. These in turn funnel urine into the renal pelvis, a central cavity that connects to the ureter, allowing urine to flow out of the kidney and toward the bladder.
Ureters, Urinary Bladder, and Urethra
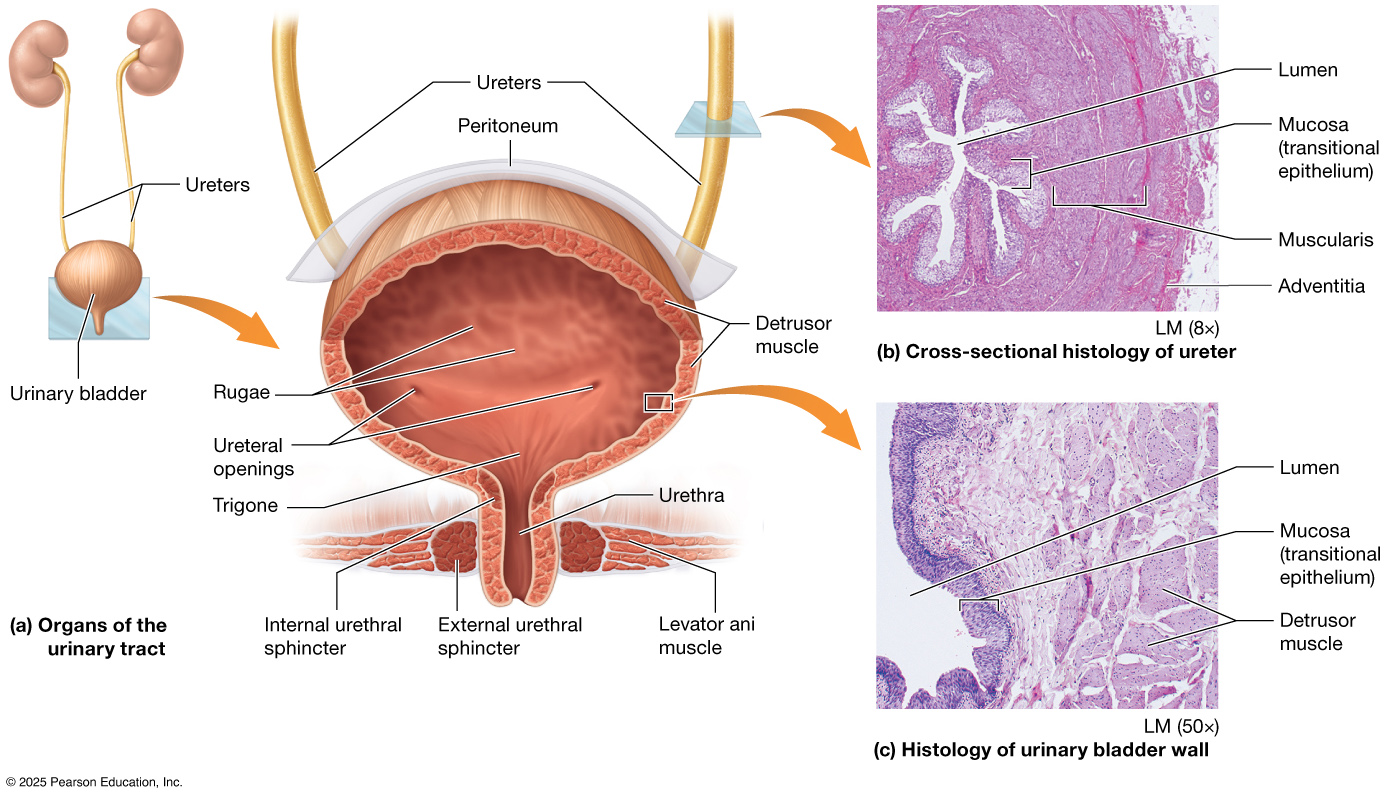
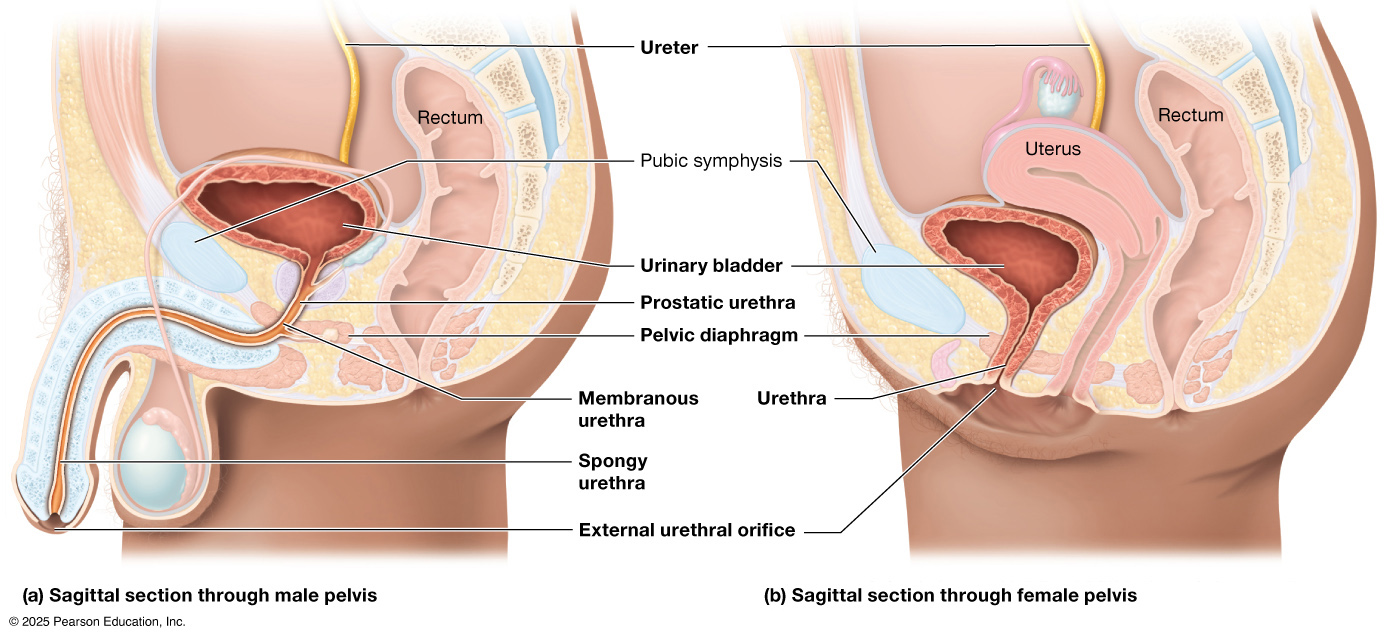
The ureter, urinary bladder, and urethra work together to transport, store, and eliminate urine from the body. Each ureter is a narrow muscular tube that carries urine from the kidneys to the urinary bladder through rhythmic contractions called peristalsis. The urinary bladder is a hollow, expandable organ that stores urine until it is ready to be excreted; it is lined with transitional epithelium (also called urothelium), a specialized tissue that can stretch to accommodate changing volumes of urine. Surrounding the bladder is the detrusor muscle, a thick layer of smooth muscle that contracts during urination to expel urine. When the bladder empties, urine passes through the urethra, a tube that carries it out of the body.
Nephron
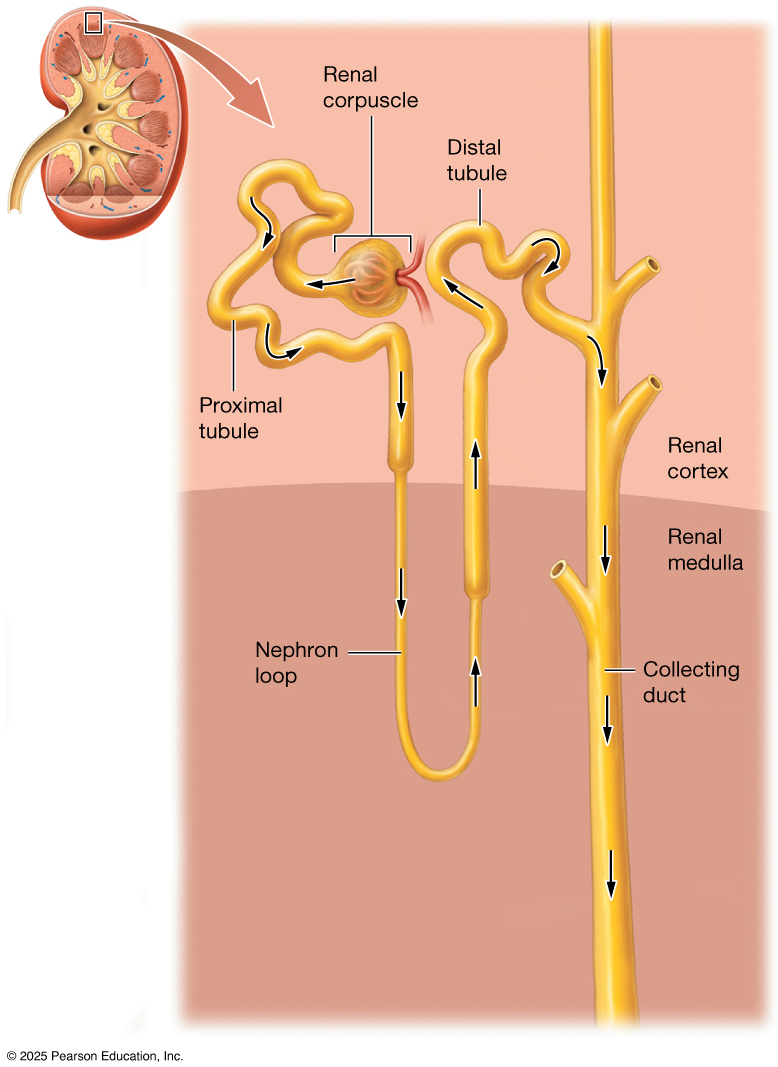
The nephron is the microscopic functional unit of the kidney, responsible for filtering blood and forming urine through a series of specialized structures. Each nephron begins with a filtration component called the renal corpuscle, made up of the glomerulus and Bowman’s capsule, where blood plasma is filtered to remove waste and excess substances. The filtrate then travels through a series of tubules — the proximal convoluted tubule, loop of Henle, and distal convoluted tubule — where essential water, ions, and nutrients are reabsorbed back into the bloodstream, while additional wastes are secreted into the fluid. Finally, the processed fluid enters a collecting duct, where its final composition is adjusted before becoming urine, allowing the nephron to play a key role in maintaining fluid balance, electrolyte levels, and overall homeostasis.
Renal Corpuscle
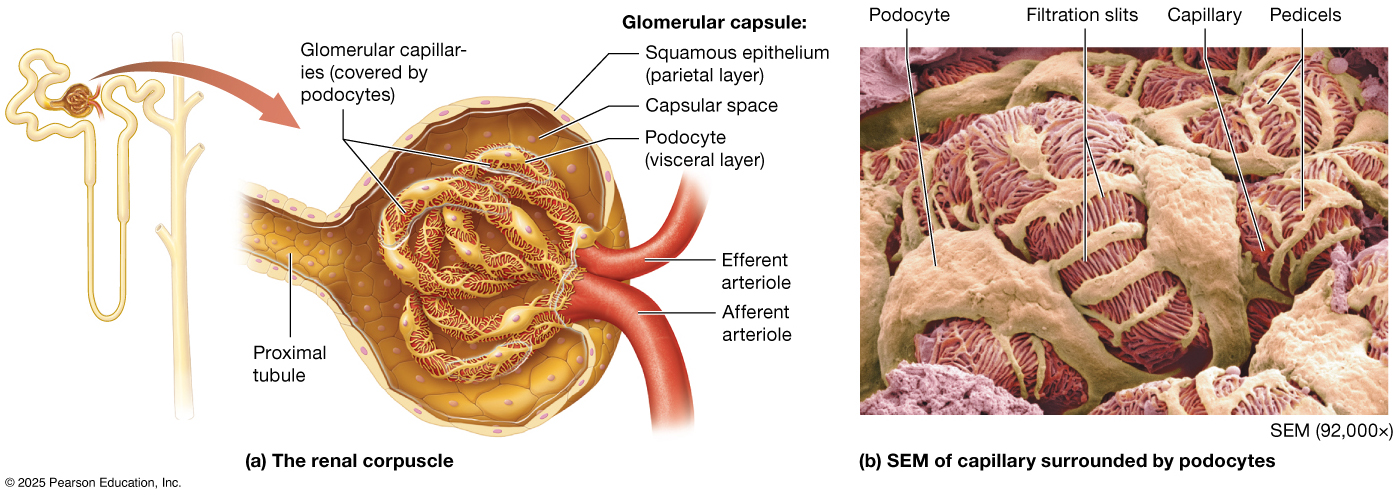
The renal corpuscle is a highly specialized structure that carries out the first step of urine formation — filtration of blood plasma. It is composed of the glomerulus, a dense network of fenestrated capillaries, enclosed by Bowman’s capsule (also called the glomerular capsule), which has two layers: a parietal layer made of simple squamous epithelium and a visceral layer formed by specialized cells called podocytes. These podocytes extend foot-like processes that interlock around the glomerular capillaries, creating narrow filtration slits that, along with the capillary endothelium and basement membrane, form a selective filtration barrier. This barrier allows water, ions, glucose, and small solutes to pass while restricting larger proteins and blood cells. Between the two layers of Bowman’s capsule is the capsule space, where filtrate collects before entering the nephron.
Blood enters the glomerulus at the vascular pole through the afferent arteriole, whose relatively larger diameter helps generate the high hydrostatic pressure needed for filtration, and exits via the narrower efferent arteriole, maintaining this pressure gradient. The resulting filtrate leaves at the urinary pole, where it enters the proximal convoluted tubule.
Proximal Convoluted Tubule
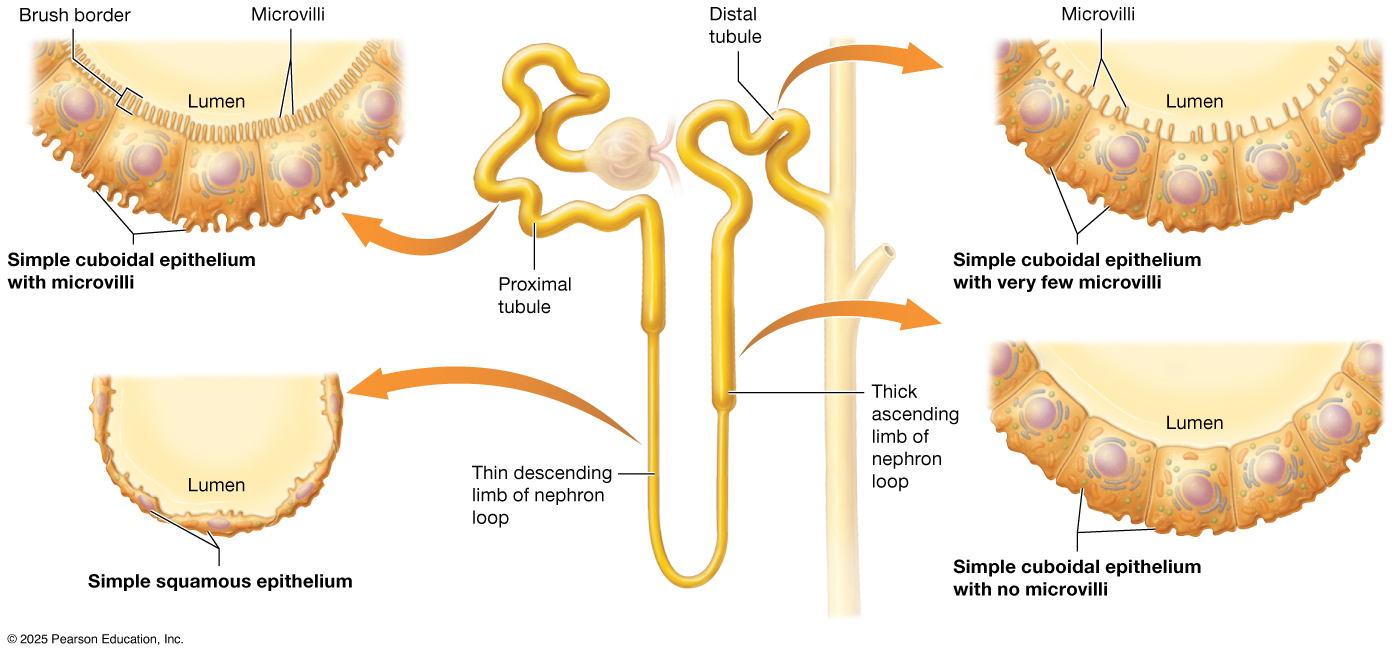
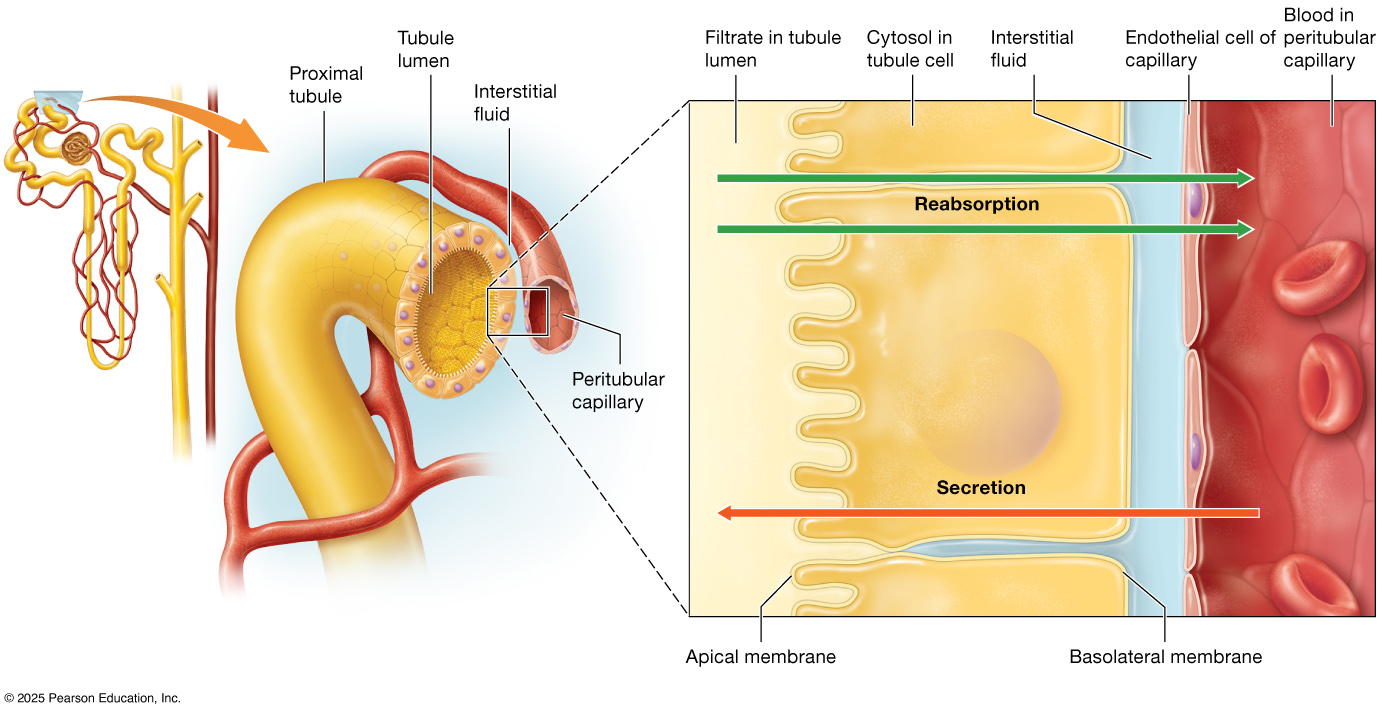
The proximal convoluted tubule is the first tubular segment of the nephron after the renal corpuscle and is primarily responsible for the reabsorption of the majority of filtered substances. Located in the cortical labyrinth of the kidney, it is closely associated with a network of peritubular capillaries that allow reabsorbed materials to quickly return to the bloodstream. The proximal convoluted tubule is lined with simple cuboidal epithelium and has a dense brush border made of microvilli, greatly increasing surface area to maximize reabsorption of water, glucose, amino acids, ions, and other essential solutes. This segment plays a critical role in reclaiming about two-thirds of the filtrate before it moves deeper into the nephron.
In histological sections, the proximal convoluted tubule appears pinker and typically has fewer visible nuclei per tubule cross-section than the distal convoluted tubule; the brush border also gives its lumen a “fuzzy” appearance.
Loop of Henle
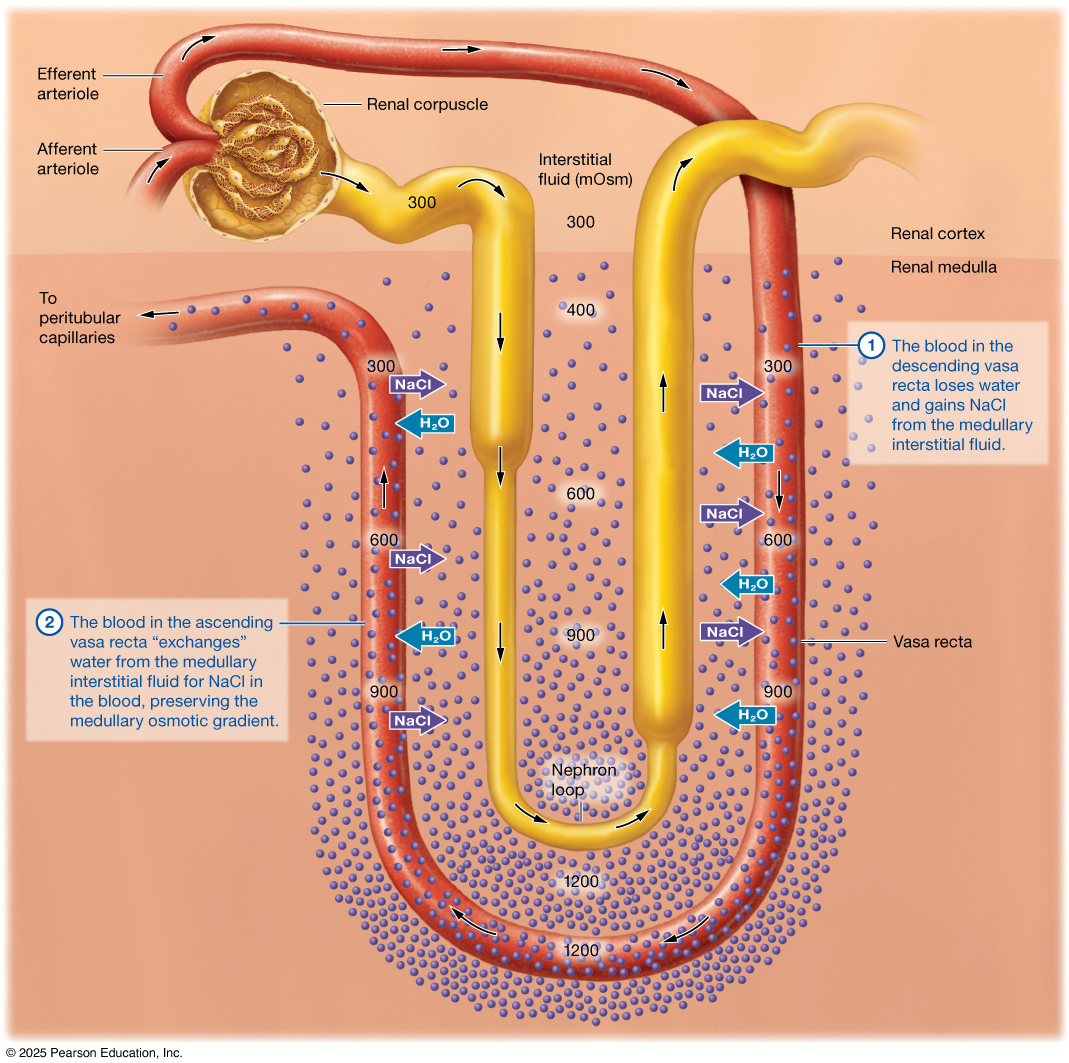
The loop of Henle is a hairpin-shaped segment of the nephron that extends from the proximal convoluted tubule in the cortex down into the medulla and then back up toward the distal convoluted tubule, forming a distinct descending limb and ascending limb. The descending limb is thin and is primarily lined with simple squamous epithelium, remaining highly permeable to water but not to solutes. The ascending limb includes both a thin portion (also simple squamous epithelium) and a thicker portion lined with simple cuboidal epithelium closer to the cortex. The thick ascending limb actively transports ions out of the filtrate but is impermeable to water.
Closely associated with the loop is the vasa recta, a series of straight capillaries that mirror the loop’s shape and run alongside it through the medulla. This parallel arrangement supports a medullary osmotic gradient that is critical for concentrating urine.
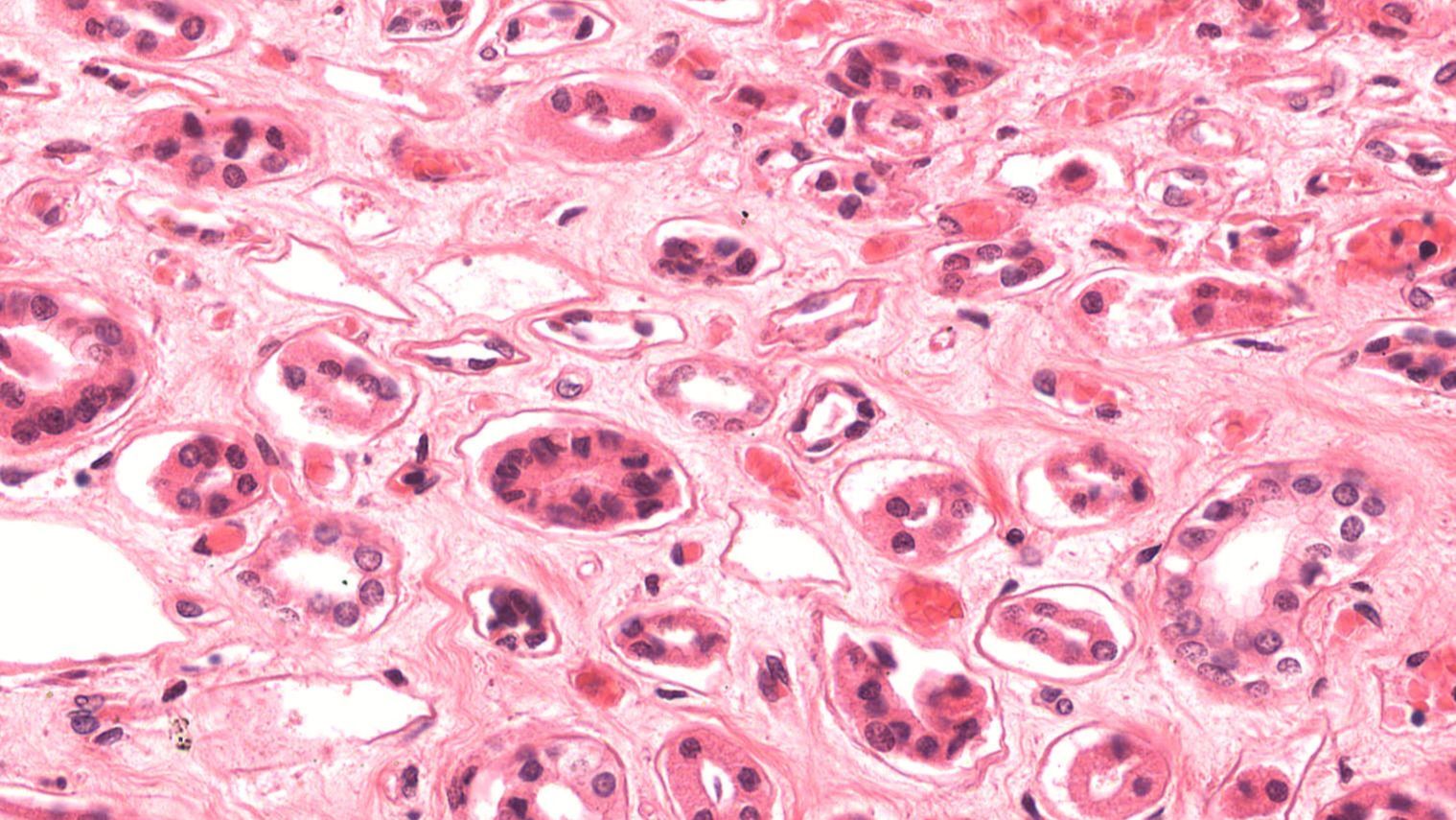
Distal Convoluted Tubule
The distal convoluted tubule is a segment of the nephron located in the cortical labyrinth that follows the loop of Henle and plays a key role in the selective regulation of electrolytes and pH. It is lined with simple cuboidal epithelium but has far fewer microvilli than the proximal convoluted tubule, reflecting its more targeted reabsorption and secretion functions. In histological sections, the distal convoluted tubule appears more purple/lighter in color and typically has more visible nuclei per cross-section than the proximal convoluted tubule due to the absence of a brush border.
A specialized region of the distal convoluted tubule, known as the macula densa, is found where the tubule comes into close contact with the afferent arteriole of its own renal corpuscle. The macula densa consists of densely packed epithelial cells that monitor the concentration of sodium and chloride in the filtrate and help regulate blood flow and filtration rate through a feedback mechanism, playing an essential role in maintaining stable glomerular filtration and blood pressure.
Collecting Ducts
The collecting ducts are the final tubular structures of the nephron system, responsible for transporting urine from multiple distal convoluted tubules to the renal pelvis. They begin in the cortical labyrinth and descend through the medulla, merging with other collecting ducts along the way to form progressively larger ducts that ultimately empty into the minor calyces. The walls of the collecting ducts are lined with simple cuboidal to columnar epithelium, which includes principal cells that regulate water and sodium reabsorption and intercalated cells that manage acid-base balance. As filtrate passes through these ducts, water reabsorption is finely adjusted under the influence of hormones such as antidiuretic hormone (ADH), concentrating the urine before it empties into the minor calyces.
Urinary System Word Bank
Essential
- afferent arteriole
- Bowman's capsule / glomerular capsule
- collecting duct
- cortex
- distal convoluted tubule
- efferent arteriole
- glomerulus
- hilum
- kidney
- loop of Henle
- major calyces
- medulla
- minor calyces
- nephron
- peritubular capillaries
- proximal convoluted tubule
- renal artery
- renal capsule
- renal columns
- renal corpuscle
- renal pelvis
- renal pyramids
- renal vein
- simple cuboidal epithelium
- simple squamous epithelium
- transitional epithelium
- ureter
- urethra
- urinary bladder
- vasa recta
Advanced
- ascending limb
- cortical labyrinth
- descending limb
- detrusor muscle
- macula densa
- retroperitoneal
- urinary pole
- vascular pole
Mastery
- brush border
- fenestrated capillary
- podocytes